Combination Therapy: Why Mixing Medicines Can Work Better
If you’ve ever heard a doctor say, “We’ll combine these two drugs,” they’re talking about combination therapy. It’s simply the practice of using two or more medications together to tackle a health problem from different angles. The idea is that each drug does something the other can’t, so together they give a stronger, quicker, or safer result.
Think of it like a sports team. One player might be fast, another strong, and a third has great strategy. When they work together, they beat the competition more easily than any single player could. The same principle applies to medicines – one drug can lower blood pressure while another eases inflammation, making the overall treatment smoother.
Why Doctors Choose Combination Therapy
Doctors often turn to combos for three main reasons:
- Better effectiveness. Some conditions, like high blood pressure or HIV, need more than one mechanism of action. Pairing an ACE inhibitor with a calcium‑channel blocker can control pressure better than either alone.
- Lower side‑effects. Using lower doses of two drugs may reduce the chance of any single drug causing trouble. For example, combining low‑dose aspirin with a blood thinner like clopidogrel (Plavix) balances clot prevention and bleeding risk.
- Convenience. Fixed‑dose combo pills let patients take one tablet instead of several, which improves adherence. A common combo is the ARB plus a diuretic for hypertension.
Real‑world examples from our site include the Lisinopril alternatives article that talks about swapping lisinopril for an ARB or CCB, often in combination with a thiazide. Another piece on Jardiance vs Glipizide highlights how adding a SGLT2 inhibitor to standard diabetes meds can boost heart health while trimming weight.
Tips for Managing Multiple Medications Safely
Mixing medicines works best when you stay organized. Here are practical steps:
- Keep a master list. Write down every drug, dose, and timing. Include over‑the‑counter pills and supplements like the popular celery supplement.
- Watch for interactions. Some combos can cause problems – mixing certain antibiotics with antacids, for instance. Use pharmacy tools or ask your pharmacist to double‑check.
- Follow the schedule. Set alarms or use a pill organizer. Missing doses can tip the balance and make the combo less effective.
- Know the side‑effects. If you start feeling dizzy, rash, or unusual bleeding, note which drug you just took and tell your doctor right away.
- Talk to your provider before adding anything. Even “natural” supplements can interfere with prescription combos. Your doctor should approve every addition.
When traveling, the Packing Medications for International Travel guide is a handy checklist – it reminds you to keep meds in original containers, carry copies of prescriptions, and check customs rules.
Bottom line: combination therapy can boost outcomes, cut side‑effects, and simplify daily routines, but it only works when you stay on top of what you’re taking. Keep your list updated, ask questions, and use tools like pharmacy counseling to keep the combo safe and effective.
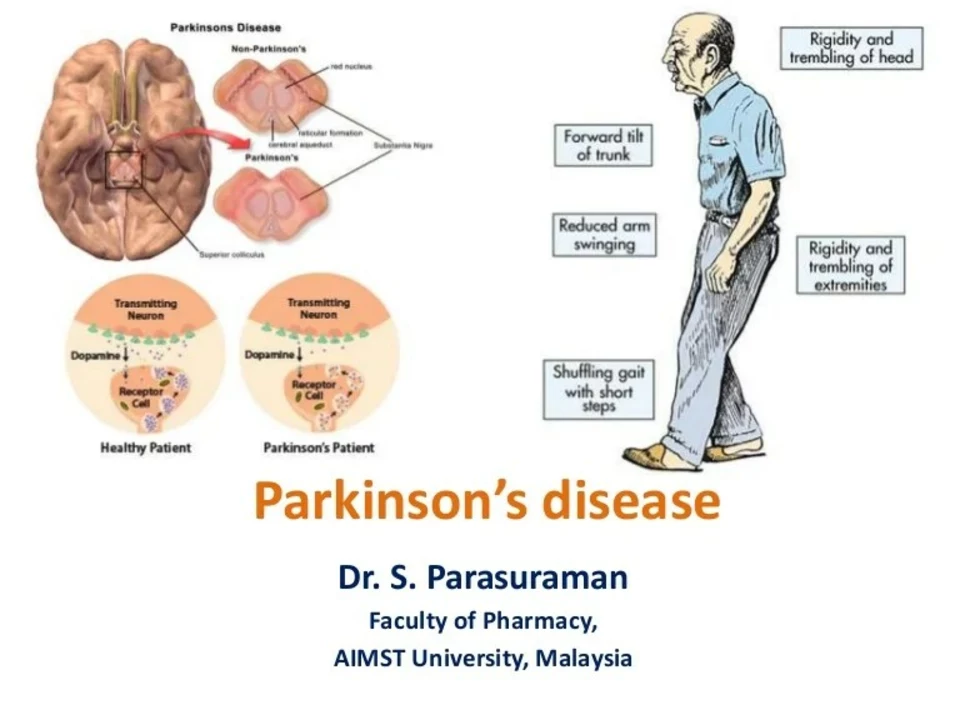
The use of Amantadine in combination with other medications for Parkinson's disease
In my recent research, I discovered that Amantadine, an antiviral medication, has shown promising results when combined with other medications to treat Parkinson's disease. This combination therapy helps alleviate symptoms such as tremors, stiffness, and difficulty with movement. Studies have revealed that Amantadine works by increasing dopamine levels in the brain, which is crucial for patients with Parkinson's. Furthermore, it has been found to have fewer side effects compared to other treatments, making it a more tolerable option for many patients. In conclusion, the use of Amantadine in combination with other medications presents a promising approach to managing Parkinson's disease symptoms and improving the quality of life for those affected.
View More