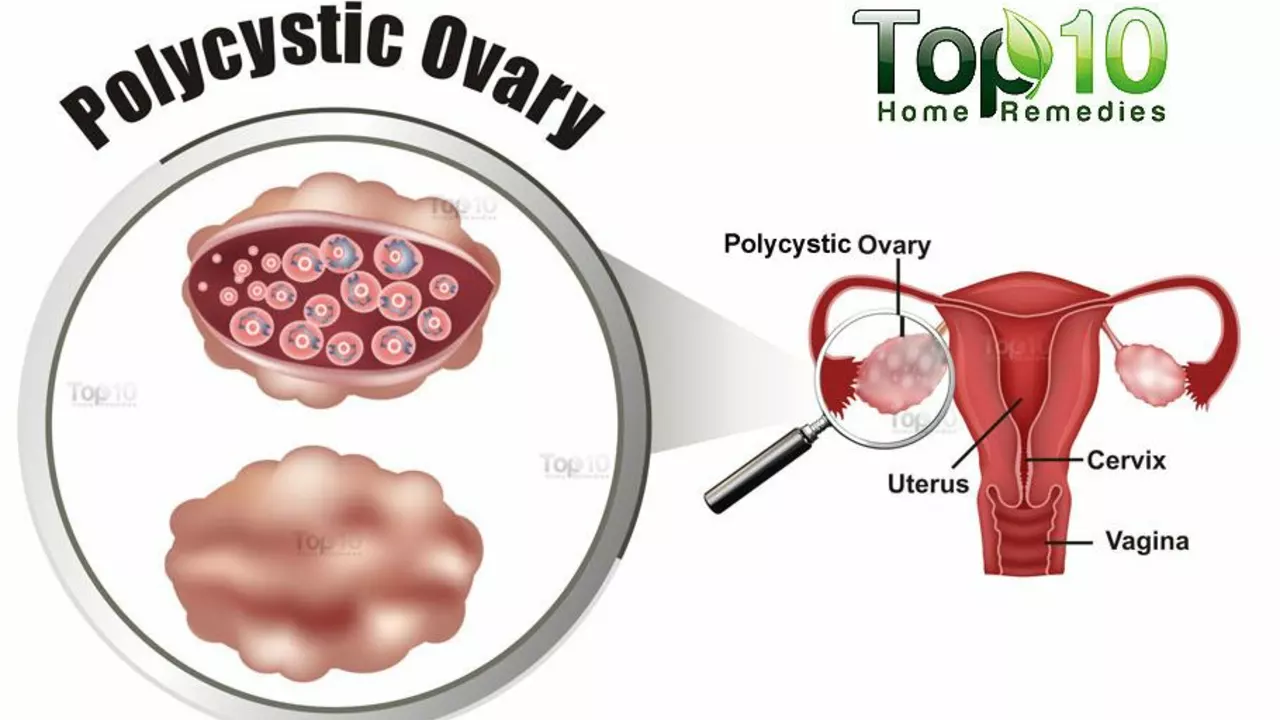
Polycystic Ovary Syndrome (PCOS): What You Need to Know
If you’ve heard the term PCOS thrown around in health blogs or doctor’s offices, you’re probably wondering what it actually means. In plain language, polycystic ovary syndrome is a hormonal imbalance that affects many people assigned female at birth, typically during their teen years or early adulthood. It shows up as irregular periods, extra hair growth, acne, and sometimes difficulty getting pregnant.
What Triggers PCOS?
The exact cause isn’t pinned down to a single factor, but most experts point to three main contributors: insulin resistance, excess androgen (male‑type hormones), and genetics. When the body’s cells don’t respond well to insulin, the pancreas pumps out more of it. High insulin can tell the ovaries to produce more androgens, which then disrupt the menstrual cycle. If a close family member has PCOS, you’re more likely to develop it too.
Because these pieces interact, symptoms can look different from person to person. Some people notice only a few stray hairs on their chin, while others struggle with weight gain and severe acne. That’s why a personalized approach matters.
Practical Ways to Manage PCOS
Good news: lifestyle tweaks can make a big dent in the toughest PCOS symptoms. Here are three easy actions you can start today:
- Move More, Eat Smarter: Aim for at least 150 minutes of moderate exercise each week—think brisk walks, cycling, or dancing. Pair that with a low‑glycemic diet (lots of veggies, whole grains, lean protein) to keep blood sugar steady.
- Watch Your Weight: Even a modest 5‑10% drop in body weight can improve insulin sensitivity and restore more regular periods. Small, consistent changes beat drastic crash diets every time.
- Talk About Medication: Doctors may prescribe birth control pills to regulate cycles, anti‑androgen meds for hair loss, or metformin to boost insulin response. These aren’t one‑size‑fits‑all, so discuss side effects and goals with your provider.
If fertility is a concern, treatments like letrozole or clomiphene can help trigger ovulation. Many people also benefit from seeing a nutritionist who specializes in PCOS—they can tailor meal plans that keep cravings low and energy high.
Beyond the big changes, don’t overlook small habits: get enough sleep, manage stress through meditation or hobbies, and stay hydrated. Each of these factors influences hormone balance subtly but consistently.
Remember, PCOS is a chronic condition, not a quick fix. Patience and steady effort are your best allies. Track symptoms in a journal; note how foods, workouts, or sleep affect your cycle. Over time you’ll see patterns that guide smarter choices.
If you’re feeling overwhelmed, reach out to support groups—online forums, local meet‑ups, or counseling can provide encouragement and practical tips from people walking the same path.
Bottom line: polycystic ovary syndrome may feel like a puzzle, but with the right pieces—balanced diet, regular movement, medical guidance—you can gain control over symptoms and improve overall health.
The Role of Alfacalcidol in Managing Polycystic Ovary Syndrome (PCOS)
Alright folks, let's talk about a not-so-funny but crucial topic - Polycystic Ovary Syndrome (PCOS). Now, who would've thought that Alfacalcidol (let's call it the 'Vitamin D rockstar') could play a role in managing this, huh? Well, it does! Alfacalcidol has been strutting its stuff, helping to regulate insulin resistance, one of the main culprits behind PCOS. Ladies, it's time we give a standing ovation to this Vitamin D rockstar for its role in helping to control those pesky PCOS symptoms.
View More